
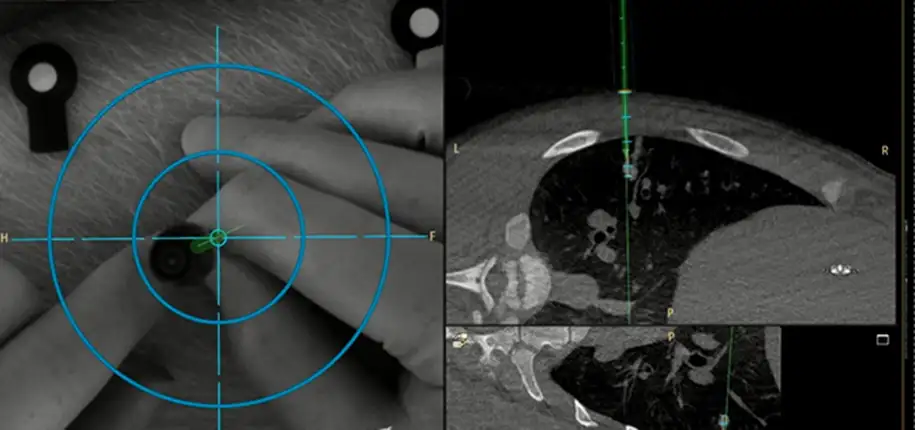
Interventional radiologists use imaging such as x-rays, CT scanning, MRI scanning and Ultrasound to guide needles and catheters (thin tubes) while performing minimally invasive procedures such as biopsies, angiograms, tumor ablations, and injections of medications or contrast. Augmented reality is a technology that superimposes (places one image over another) a computer-generated image on a real-world environment.
Researchers in the Interventional Radiology Research and Simulation Lab (IR-TRSL)are using AR technology developed by Philips Healthcare to display and track a digital image of their needle as it is advanced through a phantom or simulated patient. The augmented reality system also overlays images from a CT or MRI of the simulated patient onto a large monitor display so that the digital image of the needle can be advanced to its intended target while avoiding nearby vital structures. The interventional radiology researchers have teamed up with their surgery colleagues to practice using the augmented reality system for spine surgery (the placement of sacral nerve stimulators) and the localization and removal of lung tumors. There are so many more possibilities we have yet to utilize.
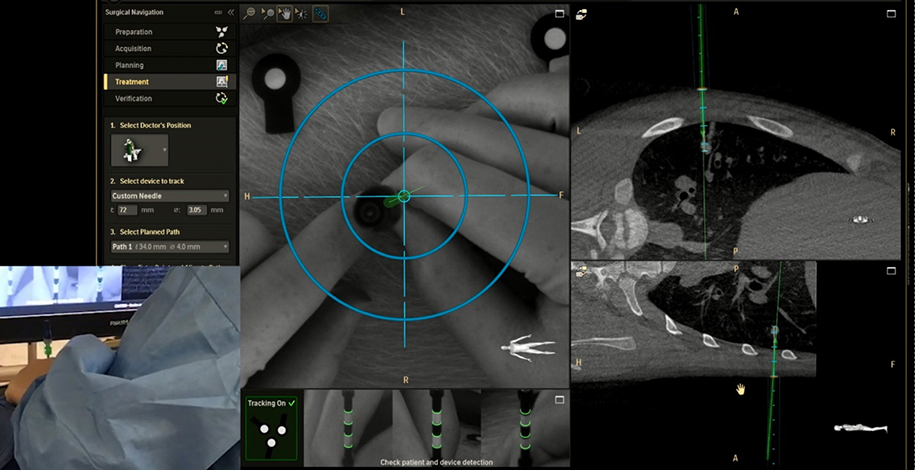
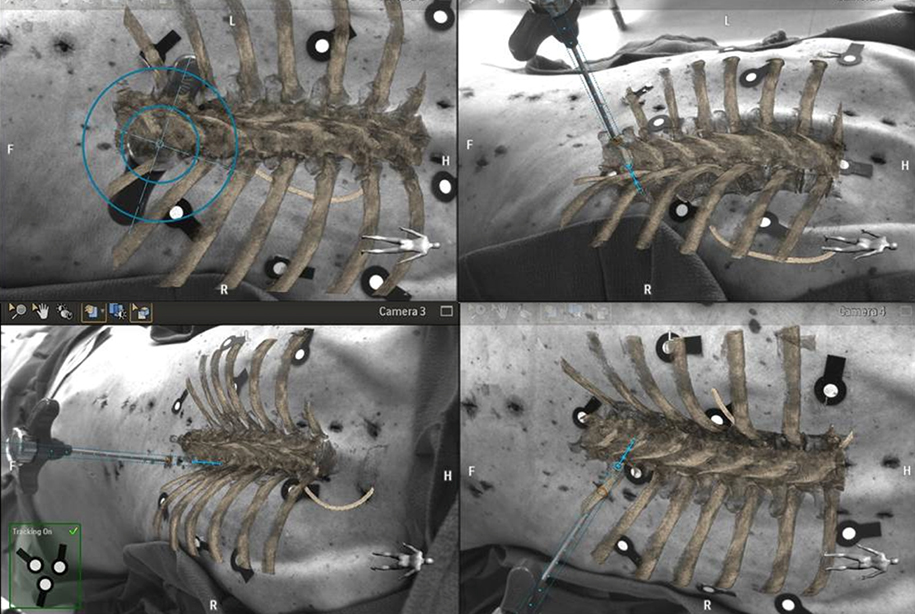
This augmented reality technology should be approved by the FDA for clinical use in 2020. Once approved, the technology will immediately be available for interventional radiologists and surgeons to use in our Hybrid operating room here at Cincinnati Children’s. What does all of this mean for patients? This augmented reality technology will enhance some current interventional radiology techniques and image-guided surgery procedures, making them more precise, safer, and less invasive overall.
Contributed by Dr. John Racadio and edited by Tony Dandino, RT(MR).
