This year I had the opportunity to develop a machine learning model to predict small bowel Crohn’s disease using magnetic resonance images (MRI) under the guidance of Jonathan Dillman, MD, Hailong Li, PhD, and Lili He, PhD, at Cincinnati Children’s Radiology. I would love to share our work with you.
Crohn’s disease is a chronic inflammation of the intestines that can come and go over time. Crohn’s affects an estimated 750,000 children and adults in the United States and is becoming more common1. Timely diagnosis in children helps lead to earlier treatment and fewer complications, such as malnutrition and impaired growth2.
While MRI is widely used to evaluate patients with suspected Crohn’s, research has demonstrated variability in MRI interpretations, even among expert radiologists3,4. Furthermore, due to the limited availability of expert pediatric abdominal radiologists, not all MRI for Crohn’s in children is interpreted by experts. When interpreted by non-experts, there is an increased chance of making the wrong diagnosis.
There is increasing research that machine learning evaluation of medical images can improve how well we diagnose many diseases. We aimed to develop a machine learning model to predict Crohn’s in pediatric patients using non-contrast MRI images. Our study included 135 patients that had a previous MRI for suspected Crohn’s. Their average age was 15 years; 50% were girls, and 70 had Crohn’s while 65 did not.
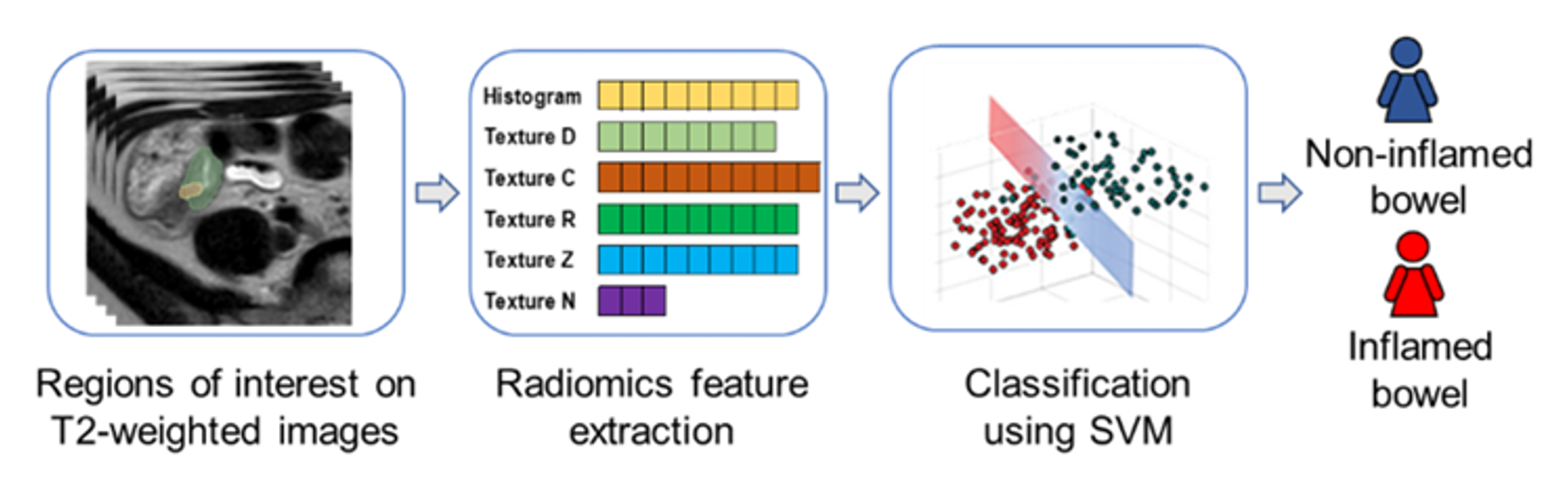
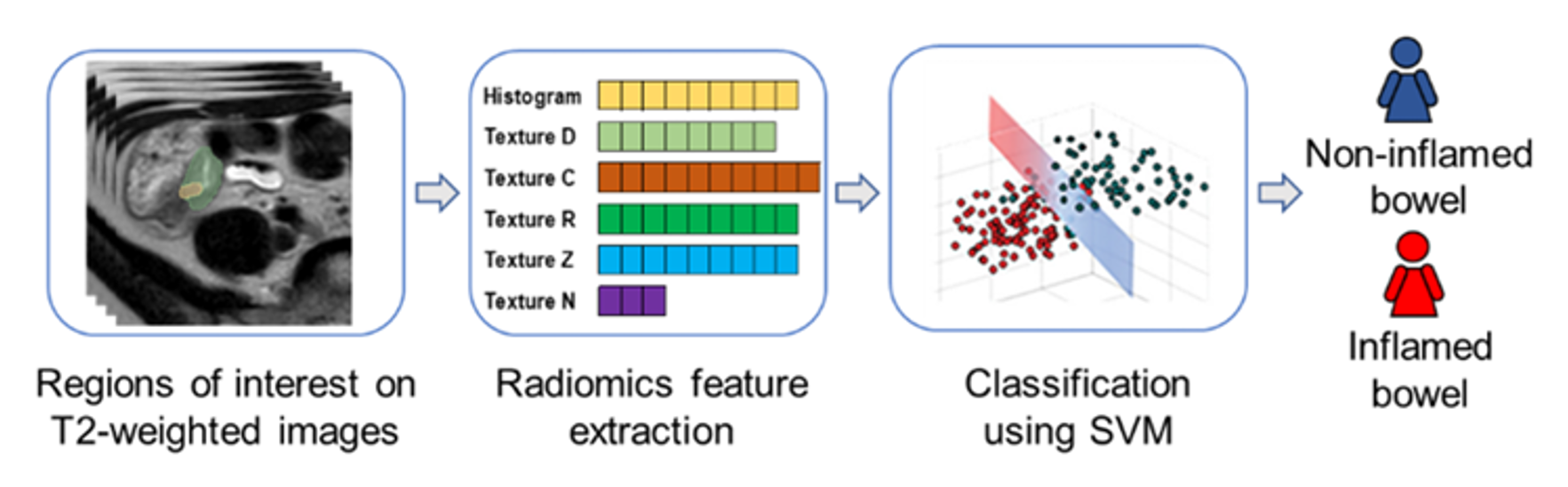
For our models, I worked with Dr. Dillman to first identify particular bowel loops. From these bowel loops, we extracted “radiomic” features related to shape, brightness, and texture. I then worked with Dr. Li to develop machine learning models to classify images as either being from a patient with Crohn’s or from a patient without Crohn’s. Our model had an accuracy of 89.5%, which was slightly better than the literature-documented accuracy of radiologists4. It is noteworthy that radiologists look at multiple types of MRI images before and after IV contrast administration to assess disease, while our model uses only one image type.
We then developed a model for predicting Crohn’s using routinely collected data, like weight, age, and laboratory testing. We combined this model with our imaging model to achieve an excellent diagnostic accuracy of 93.5% for diagnosing Crohn’s.
We believe that this model has the potential to improve our ability to diagnose Crohn’s in children and decrease the variability in diagnosis between radiologists. However, while our results are promising, future multi-center studies are needed. We hope to use similar methods to investigate other key clinical questions in Crohn’s management, including determining if images from diagnosis predict response to certain medical therapies, the development of future complications, and the need for future surgery.
Figure: an overview of the machine learning method

Richard Lui, author; Glenn Miñano, BFA, editor; Meredith Towbin, copy editor